Few prenatal moments generate as much quiet anxiety as the glucose challenge test. You drink a syrupy-sweet solution, sit in a waiting room, and then wonder whether the number on your lab report means everything is fine — or whether more testing lies ahead.
This test is also called the 1-hour glucose test or 1-hour glucose screening, and it is a routine part of pregnancy care rather than an emergency test.
The good news? This routine screening is straightforward, usually painless, and gives your healthcare provider critical information about how your body handles sugar during pregnancy. Even if your results come back higher than expected, that single number does not mean you have gestational diabetes.
This guide explains exactly what the glucose challenge test involves, what the normal range looks like, how results are interpreted, and what happens next — so you can walk into your appointment informed and confident.
Table of Contents
Quick Summary
- What is it? → A one-hour blood-sugar screening done during pregnancy to check for gestational diabetes.
- When is it done? → Usually between 24 and 28 weeks of pregnancy; earlier if risk factors exist.
- Do I need to fast? → No fasting required for the standard 1-hour GCT.
- What’s normal? → A blood sugar level below 140 mg/dL (7.8 mmol/L) one hour after drinking the glucose solution.
- Failed the test? → An abnormal result triggers a follow-up 3-hour oral glucose tolerance test (OGTT); it does not by itself mean you have gestational diabetes.
What Is a Glucose Challenge Test?
The glucose challenge test (GCT) is a prenatal screening that measures how efficiently your body processes sugar. It involves drinking a 50-gram glucose solution and having your blood drawn exactly one hour later to check your blood sugar level. Exact cutoffs can vary slightly between clinics, so your provider may explain a number that is a little different from what you see online.
The GCT is a screening tool, not a diagnostic test. That distinction matters. An elevated result does not confirm gestational diabetes — it simply identifies individuals who need a longer, more detailed oral glucose tolerance test (OGTT) to reach a diagnosis.
How Does the Glucose Challenge Test Work?
During pregnancy, the placenta produces hormones that help your baby grow. Some of these hormones — particularly human placental lactogen (hPL) — make your cells less responsive to insulin. This is called insulin resistance.
For most pregnant individuals, the pancreas compensates by producing more insulin. But when the body can’t produce enough insulin to overcome placental hormone-driven resistance, blood sugar rises. The GCT checks whether that compensation is working.
Because pregnancy care can differ between regions and hospitals, your exact testing protocol may be slightly different from what is described here, and your own clinician’s instructions should always come first.
Glucose Challenge Test vs Glucose Tolerance Test — Key Differences
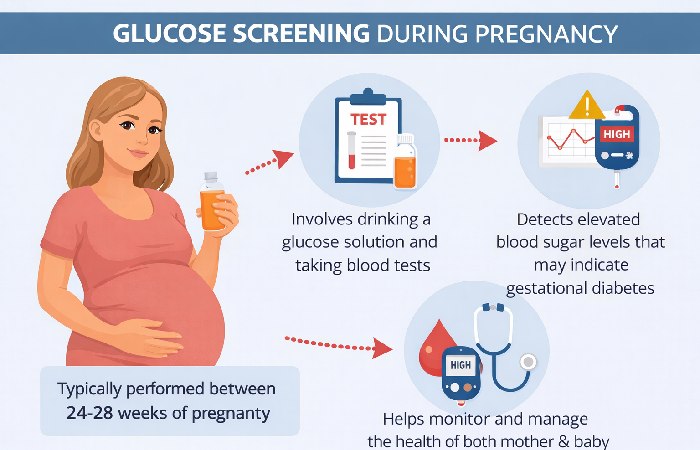
These two tests are often confused. Here’s how they compare:
| Feature | Glucose Challenge Test (GCT) | Oral Glucose Tolerance Test (OGTT) |
|---|---|---|
| Purpose | Screening | Diagnosis |
| Glucose dose | 50 g | Usually 100 g in the 3-hour test (some protocols use 75 g in a 2-hour test) |
| Fasting required? | No | Yes (8–14 hours) |
| Blood draws | 1 (at 1 hour) | 2–4 (fasting + hourly) |
| Duration | ~1 hour | 2–3 hours |
| Determines GDM? | No (screens only) | Yes (confirms or rules out) |
Think of the GCT as the initial filter and the OGTT as the definitive answer.
Why Is the Glucose Challenge Test Done During Pregnancy?
Gestational diabetes mellitus (GDM) affects roughly 2–10% of pregnancies each year, according to the CDC. It rarely causes obvious symptoms, which is why screening is the only reliable way to detect it.
Left unmanaged, GDM can lead to:
- Macrosomia — a larger-than-average baby, increasing the risk of birth injuries and cesarean delivery.
- Preeclampsia — a potentially life-threatening rise in blood pressure.
- Neonatal hypoglycemia — dangerously low blood sugar in the newborn shortly after birth.
- Higher long-term risk — both parent and child face elevated risk of developing type 2 diabetes later in life.
Screening with the GCT catches these risks early, when dietary changes, exercise, and — if necessary — medication can make a significant difference.
When Is the Test Performed?
The standard window is 24 to 28 weeks of pregnancy (second trimester). This is when placental hormones are strong enough to reveal insulin-processing problems.
If you have risk factors, your provider may schedule the GCT as early as your first prenatal visit.
Risk Factors That May Require Earlier Testing
You may be tested earlier if you have:
- A body mass index (BMI) of 30 or higher
- A history of gestational diabetes in a previous pregnancy
- A first-degree relative with type 2 diabetes
- Polycystic ovary syndrome (PCOS) or metabolic syndrome
- Age 35 or older during pregnancy
- A previous baby weighing more than 9 pounds (4.1 kg) at birth
- Belonging to a higher-risk ethnic group (Black, Hispanic, American Indian, Asian American)
- A sedentary lifestyle
If your early test comes back normal, expect a second screening at the standard 24–28-week window.
How to Prepare for the Glucose Challenge Test
Preparation is minimal, which is one reason the GCT is so widely used.
Do You Need to Fast?
No. The standard 1-hour GCT does not require fasting. You can eat and drink normally before your appointment.
NOTE
Do not confuse this with the 3-hour OGTT, which does require 8–14 hours of fasting. Your provider will give specific instructions if you need the follow-up test.
What to Eat Before the Glucose Challenge Test
While fasting isn’t required, a few practical tips can help you feel more comfortable:
- Eat a balanced meal 1–2 hours before the test (protein, healthy fats, complex carbs).
- Avoid loading up on simple sugars (candy, soda, pastries) immediately beforehand — while this won’t invalidate the test, it may amplify nausea.
- Stay hydrated with water.
- Inform your provider about any medications you’re taking, as some drugs can affect blood sugar readings.
Glucose Challenge Test Procedure — Step by Step

Here’s exactly what to expect on test day:
- Arrive at the lab or clinic. No special check-in is needed beyond a standard appointment.
- Drink the glucose solution. You’ll receive a sweet drink (often called “glucola”) containing 50 grams of glucose. It tastes like a very sweet soda or flat orange drink. You’ll need to finish it within about 5 minutes.
- Wait one hour. Sit in the waiting area. You cannot eat or drink anything other than small sips of water during this period. Bring a book, phone, or podcast.
- Blood draw. A phlebotomist draws blood from a vein in your arm at the one-hour mark.
- Resume normal activities. You can eat, drink, and go about your day immediately after the draw.
Results are typically available within 1–3 business days. Your provider will contact you with the outcome.
Possible side effects of the glucose drink:
- Mild nausea
- Dizziness or lightheadedness
- A “sugar rush” followed by a crash
- Headache
These are temporary and usually resolve within a few hours. If you vomit during the waiting period, notify the lab staff — the test may need to be repeated.
Glucose Challenge Test Normal Range and Results
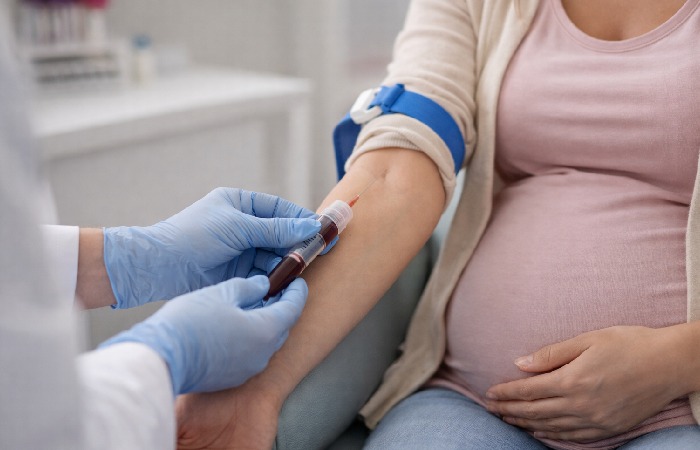
This is the section most readers need. Let’s break down the numbers clearly.
1-Hour GCT Normal Values
| Result | Interpretation |
|---|---|
| Below 140 mg/dL (7.8 mmol/L) | Normal — no further testing needed |
| 140–189 mg/dL (7.8–10.5 mmol/L) | Abnormal — 3-hour OGTT recommended |
| 190 mg/dL (10.6 mmol/L) or higher | Strongly suggestive of GDM — your provider may recommend closer monitoring and will usually confirm with further testing or clinical judgment |
IMPORTANT: Some clinics use a lower threshold of 130 mg/dL (7.2 mmol/L) to cast a wider screening net. Always defer to your provider’s specific cutoff.
3-Hour OGTT Normal Values (Carpenter-Coustan Criteria)
If your GCT result is abnormal, the follow-up OGTT uses a 100 g glucose load and multiple blood draws:
| Time Point | Normal Threshold |
|---|---|
| Fasting | Below 95 mg/dL (5.3 mmol/L) |
| 1 hour | Below 180 mg/dL (10.0 mmol/L) |
| 2 hours | Below 155 mg/dL (8.6 mmol/L) |
| 3 hours | Below 140 mg/dL (7.8 mmol/L) |
Diagnosis rule: If two or more values meet or exceed these thresholds, gestational diabetes is diagnosed.
Some clinicians may follow slightly different diagnostic criteria based on regional or institutional guidelines, so your report may look a little different while still being evidence-based.
What Happens If You Fail the Glucose Challenge Test?
First, take a breath. The word “fail” is misleading. An abnormal screening result means your body’s initial response to sugar warrants a closer look — nothing more.
Understanding an Abnormal Result
Roughly 15–25% of women who take the GCT receive a result above the cutoff. Of those, only a portion are ultimately diagnosed with gestational diabetes after the OGTT, so many “failures” turn out not to have GDM.
Next Steps — The 3-Hour OGTT
If your 1-hour GCT result is elevated:
- Your provider will schedule a 3-hour oral glucose tolerance test.
- You’ll need to fast for 8–14 hours before the OGTT.
- A fasting blood sample is drawn first.
- You drink a higher-dose glucose solution (usually 100 g for the 3-hour test; in some protocols 75 g is used for a 2-hour test).
- Blood is drawn at 1-hour, 2-hour, and 3-hour intervals.
- Results are compared against established thresholds to confirm or rule out GDM.
Understanding the DIPSI Method (75 g Single-Step Test)
In several countries — particularly India — the DIPSI (Diabetes in Pregnancy Study Group India) protocol is used as an alternative to the two-step Western approach.
How it differs:
- Uses a 75 g glucose load (not 50 g).
- Does not require fasting — the drink is taken regardless of meal timing.
- Blood is drawn 2 hours after consumption.
- A result of ≥140 mg/dL at the 2-hour mark indicates gestational diabetes.
The DIPSI method is a single-step screening-and-diagnosis test, meaning there’s no separate confirmatory OGTT. It’s designed for resource-limited settings where follow-up testing access is challenging, as recommended by the WHO’s diagnostic criteria for gestational diabetes.
Risks and Complications of Gestational Diabetes
If the GCT and subsequent OGTT confirm GDM, timely management is essential. Unmanaged gestational diabetes can lead to:
- For the baby: Macrosomia (large birth weight), respiratory distress, neonatal jaundice, low blood sugar after birth, and increased future risk of obesity and type 2 diabetes.
- For the parent: Preeclampsia, increased likelihood of cesarean delivery, and a higher long-term risk of developing type 2 diabetes (in some studies, up to about half may develop it within 5–10 years).
These risks are significantly reduced with proper management, which typically involves blood-sugar monitoring, dietary changes, regular physical activity, and — when necessary — insulin or oral medication.
Common Mistakes and Misconceptions About the Glucose Test
- “I failed, so I have gestational diabetes.” Not true. The GCT is a screening, not a diagnosis. Many women pass the follow-up OGTT.
- “I can eat extra sugar to ‘train’ my body before the test.” This has no proven benefit and may increase nausea.
- “Fasting before the 1-hour test will give better results.” Fasting isn’t required and can cause lightheadedness. Eat normally.
- “Gestational diabetes means I did something wrong.” GDM is driven by placental hormones, not personal habits. It can happen to anyone.
- “If I had a normal result, I’m in the clear forever.” A normal GCT at 24–28 weeks doesn’t guarantee you won’t develop glucose issues later. Follow your provider’s complete care plan.
Who Should Take & Who May Need Extra Attention
Best for:
- All pregnant individuals between 24–28 weeks as part of standard prenatal care.
- Those with no prior pregnancy complications seeking routine screening.
Extra attention needed for:
- Individuals with BMI ≥30, PCOS, or metabolic syndrome.
- Anyone with a history of GDM in a prior pregnancy.
- Those with a family history of type 2 diabetes.
- Individuals aged 35+ during pregnancy.
If you fall into the higher-risk group, don’t wait until 24 weeks — talk to your provider about earlier screening.
Postpartum Follow-Up — Why It Matters
Many people assume the glucose conversation ends once the baby arrives. It doesn’t.
The American College of Obstetricians and Gynecologists (ACOG) recommends that individuals diagnosed with gestational diabetes undergo a 2-hour, 75 g OGTT between 4 and 12 weeks postpartum to screen for type 2 diabetes.
Why this matters:
- Studies suggest that a significant number of individuals with GDM go on to develop type 2 diabetes within about 10 years if no preventive steps are taken.
- Early detection through postpartum testing allows for lifestyle interventions that can delay or prevent progression to type 2 diabetes.
- Breastfeeding, balanced nutrition, and regular physical activity after delivery can help normalise blood sugar.
Despite its importance, postpartum glucose testing is frequently skipped. If you had GDM, make this follow-up a priority.
Final Verdict
The glucose challenge test is one of the most valuable prenatal screenings available. It’s quick, requires no fasting, and gives your healthcare team essential information about your metabolic health during pregnancy.
If your result is normal — great. If it’s elevated, remember: an abnormal screening is not a diagnosis. The follow-up OGTT will give a clearer picture. And even if gestational diabetes is confirmed, it is highly manageable with the right support.
Stay informed, stay proactive, and make sure to follow through on postpartum testing if recommended.
Always discuss your specific numbers and next steps with your own healthcare provider, because they know your medical history and local guidelines best.
Frequently Asked Questions
Q1: What is the normal range for a glucose challenge test?
A blood sugar level below 140 mg/dL (7.8 mmol/L) one hour after drinking the 50 g glucose solution is considered normal. Some clinics use a stricter cutoff of 130 mg/dL.
Q2: Do you have to fast for the glucose challenge test?
No. The standard 1-hour GCT does not require fasting. You can eat and drink normally before the test. Fasting is only required for the follow-up 3-hour OGTT.
Q3: What happens if you fail the glucose challenge test?
An abnormal result means your blood sugar was above the screening threshold. Your provider will schedule a 3-hour oral glucose tolerance test (OGTT) to determine whether you have gestational diabetes. Many women who “fail” the GCT pass the OGTT.
Q4: What is the difference between GCT and OGTT?
The GCT (glucose challenge test) is a one-hour screening with a 50 g glucose dose and no fasting. The OGTT (oral glucose tolerance test) is a diagnostic test with a 75 g or 100 g dose, requiring fasting and multiple blood draws over 2–3 hours.
Q5: What are the side effects of the glucose drink?
Common side effects include nausea, dizziness, headache, and a sugar rush or crash. These are temporary and typically resolve within a few hours. Drinking the solution cold may help reduce nausea.
Q6: Is the glucose challenge test done in every pregnancy?
Yes. Current guidelines from ACOG recommend universal screening between 24 and 28 weeks. Earlier screening is advised for individuals with risk factors.
About Health4fitnessblog
Health4fitnessblog publishes practical, easy-to-understand content on health, technology, business, marketing, and lifestyle. Articles are based mainly on reputable, publicly available information, with AI tools used only to help research, organise, and explain topics more clearly so the focus stays on real‑world usefulness rather than jargon or unnecessary complexity.
