Every year, thousands of people across the UK wonder whether they can get gastric sleeve surgery on the NHS — and most don’t know where to start. The eligibility criteria feel confusing, the referral pathway is multi-layered, and waiting times vary wildly depending on where you live.
Here’s the good news. Gastric sleeve surgery is available completely free on the NHS for patients who meet specific criteria. But getting approved isn’t as simple as walking into your GP’s office and asking. It requires documented evidence, patience, and a willingness to commit to lifelong changes.
This guide walks you through every step — from checking your eligibility to understanding the full NHS referral pathway, realistic waiting times, and what to do if you’re turned down. Whether you’re just starting to research your options or already partway through the process, this is designed to give you clear, actionable answers.
Table of Contents
Quick Takeaways: NHS Gastric Sleeve
- Who qualifies? BMI 40+, or BMI 35–40 with obesity‑related conditions like type 2 diabetes or sleep apnoea.
- What’s the process? GP referral → Tier 3 programme (typically 6–12 months) → multidisciplinary assessment → Tier 4 surgery.
- How long is the wait? Typically 18 months to 3+ years overall, depending on your NHS region.
- Is it free? Yes, fully funded on the NHS for eligible patients.
- If you don’t qualify? Private gastric sleeve in the UK usually costs around £8,000–£12,000.
What Is Gastric Sleeve Surgery?

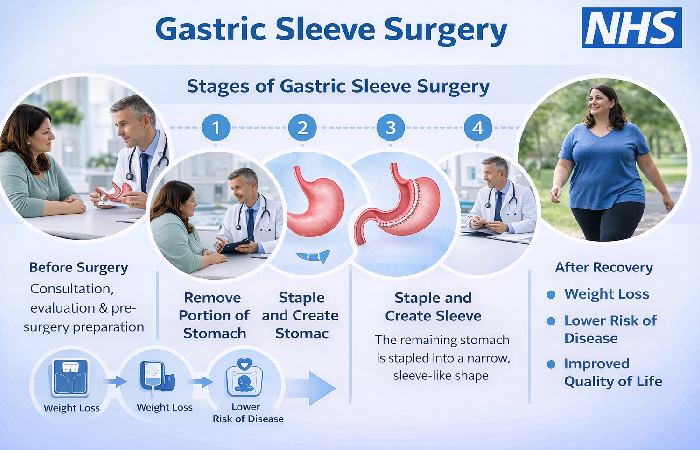
A gastric sleeve — formally known as a sleeve gastrectomy — is a surgical weight loss procedure where approximately 75–80% of the stomach is permanently removed. The remaining stomach is shaped into a narrow, banana-sized tube or “sleeve.”
The operation is performed laparoscopically (through small incisions using a camera), typically takes 1–3 hours, and usually requires a 2–3 night hospital stay.
How it works: By dramatically reducing the stomach’s capacity, the procedure limits how much food you can eat in a single sitting. It also reduces the production of ghrelin — the hormone responsible for hunger signals — which helps reduce appetite beyond just physical restriction.
Most patients lose **50–70% of their excess body weight** within 12–24 months of surgery.
Gastric Sleeve vs Gastric Bypass — Which Does the NHS Prefer?
This is a question many patients don’t think to ask until their surgical consultation. Both procedures are available on the NHS, but they work differently.
| Feature | Gastric Sleeve | Gastric Bypass |
|---|---|---|
| How it works | Removes ~80% of stomach | Creates small stomach pouch + reroutes intestine |
| Reversible? | No | Technically, but very rarely reversed |
| Surgery time | 1–2 hours | 2–3 hours |
| Weight loss (12–24 months) | 50–70% of excess weight | 60–80% of excess weight |
| Diabetes remission rate | High | Higher |
| Nutritional deficiency | Moderate | Higher (due to malabsorption) |
| Reflux risk | Higher (can worsen GORD) | Lower (often improves reflux) |
Recent research supported by the National Institute for Health and Care Research suggests that gastric bypass may be more clinically and cost-effective than sleeve gastrectomy for many patients. Your bariatric surgeon will discuss which procedure is most appropriate based on your individual health profile.
The key takeaway? Don’t set your heart on one specific procedure before your surgical consultation. Your surgeon may recommend an alternative — and that recommendation is usually based on evidence.
Who Is Eligible for Gastric Sleeve on the NHS?
NHS eligibility for gastric sleeve surgery is determined by NICE clinical guideline CG189, which sets out the criteria bariatric teams follow when assessing patients.
BMI Criteria and NICE Guidelines
You may be eligible for NHS-funded gastric sleeve surgery if you meet one of these BMI thresholds:
- BMI of 40 or above (classified as severely obese) — even without additional health conditions
- BMI between 35 and 40 — with at least one significant obesity-related health condition that could improve with weight loss
- BMI between 30 and 35 — bariatric surgery may be considered in exceptional cases, particularly if you have **recent-onset type 2 diabetes**, following specialist assessment.
!IMPORTANT: BMI alone doesn’t guarantee eligibility. You must also demonstrate that non-surgical weight management methods haven’t worked for you over at least 12 months.
Qualifying Health Conditions (Co-Morbidities)
If your BMI falls between 35 and 40, you’ll need at least one of these conditions to meet the criteria:
- Type 2 diabetes (especially recent-onset)
- High blood pressure** (hypertension)
- Obstructive sleep apnoea
- Non-alcoholic fatty liver disease (NAFLD)
- Severe osteoarthritis** significantly affecting mobility
- Heart disease
Ethnicity-Adjusted BMI Thresholds — Do You Qualify at a Lower BMI?
This is one of the most under-discussed aspects of NHS bariatric eligibility. According to NICE guidance, the standard BMI thresholds should be **reduced by 2.5 kg/m²** for people of:
- South Asian family background
- Chinese or other Asian background
- Middle Eastern background
- Black African or African-Caribbean background
This means a BMI threshold of **37.5** (instead of 40) or **32.5** (instead of 35) may apply. These adjusted thresholds exist because people from these ethnic groups tend to carry fat centrally and face higher cardiometabolic risk at lower BMI levels.
If you fall into one of these groups, make sure your GP and bariatric team apply the correct thresholds during your assessment.
The NHS Referral Pathway — Step by Step

Getting a gastric sleeve on the NHS isn’t a single appointment. It’s a structured pathway that typically takes **18 months to 3+ years** from start to finish. Here’s how it works:
Step 1 — GP Consultation and Initial Referral
Everything starts with your GP. Book an appointment specifically to discuss bariatric surgery. Your GP will:
- Check your BMI and assess whether you meet the initial criteria
- Review your medical history and any obesity-related conditions
- Refer you to a Tier 3 specialist weight management service
Practical tip: Bring documentation of any previous weight loss attempts — diet programmes, gym memberships, dietitian appointments, or medication records. This evidence strengthens your case.
Step 2 — Tier 3 Weight Management Programme (6–12 Months)
Before you can be considered for surgery, you must complete a structured Tier 3 programme. These are NHS-funded, multidisciplinary programmes that typically include:
- Dietitian consultations — personalised meal planning and nutritional guidance
- Behavioural support — understanding eating habits, triggers, and emotional eating
- Physical activity guidance — structured exercise plans appropriate for your mobility level
- Psychological assessment** — evaluating your mental readiness for surgery and long-term changes
Most programmes run for **6–12 months**, and many areas ask you to demonstrate around **5–10% weight loss** or clear behavioural changes during this period.
!NOTE: Dropping out of the Tier 3 programme — even briefly — can reset your timeline. Attend every appointment, even when progress feels slow.
Step 3 — Multidisciplinary Assessment and Surgical Referral (Tier 4)
After completing Tier 3, your weight management team will conduct a comprehensive assessment. This involves:
- A surgeon reviewing your suitability for the procedure
- A specialist nurse coordinating your care pathway
- A psychologist confirming you understand the commitment required
- A dietitian confirming you can follow post-surgery dietary requirements
If the team agrees you’re a suitable candidate, you’ll be referred to a **Tier 4 bariatric surgical service** and placed on the surgical waiting list.
Step 4 — Pre-Surgery Preparation and the Operation
Before your surgery date, you’ll typically need to:
- Follow a liver-shrinking diet (2–4 weeks of a very low-calorie diet)
- Stop smoking (if applicable — strongly advised)
- Have final blood tests and pre-operative checks
- Attend a pre-admission clinic
The operation itself is performed laparoscopically under general anaesthetic. Most patients stay in hospital for **2–3 nights** and return to normal activities within **3–6 weeks**.
How Long Is the NHS Waiting List for Gastric Sleeve?
This is where honest expectations matter. NHS waiting times for bariatric surgery are **substantial** — and they vary significantly by region.
| Stage | Typical Wait |
|---|---|
| GP consultation → Tier 3 referral | 2–4 months |
| Tier 3 programme duration | 6–12 months |
| Tier 3 completion → surgical approval | 2–6 months |
| Surgical waiting list → operation | 6–18+ months |
| Total estimated timeline | 18 months – 3+ years |
The Postcode Lottery Problem
Not all NHS regions offer the same level of bariatric access. Investigations by national newspapers have reported that budget pressures have significantly affected obesity services in many parts of England, with bariatric surgery access restricted in a large number of local areas.
What does this mean in practice? Two patients with identical BMIs and health conditions can have dramatically different experiences depending on which NHS Integrated Care Board (ICB) area they live in. Some regions have active bariatric programmes with steady throughput. Others have effectively frozen referrals.
You can check your local area’s waiting times by using the My Planned Care NHS website, and you have the legal right to ask to be referred to a different provider if waiting times are excessive.
What Happens After Surgery — Recovery and Long-Term Care

Surgery is just the beginning. Long-term success depends entirely on what happens next.
Diet and Nutrition After Gastric Sleeve
Your diet will go through several stages in the weeks following surgery:
- Week 1–2: Clear liquids only (water, broth, sugar-free jelly)
- Week 2–4: Puréed foods
- Week 4–6: Soft foods
- Week 6+: Gradual return to solid foods
Long-term, aim for **three small meals per day** rich in protein. Eat slowly, chew thoroughly, and avoid drinking during meals. Carbonated drinks and high-sugar foods are best avoided permanently.
Vitamin Supplementation and Blood Monitoring
Because your stomach is significantly smaller, your ability to absorb certain nutrients is reduced. **Lifelong vitamin supplementation is mandatory**, typically including:
- Multivitamin with iron
- Vitamin B12
- Calcium and Vitamin D
- Folic acid
You’ll also need **annual blood tests** to monitor for deficiencies. Your bariatric team will follow up for the first two years, after which your GP takes over long-term monitoring, as outlined on the NHS weight loss surgery page.
Expected Weight Loss Results
Most patients can expect to lose **50–70% of their excess body weight** within 12–24 months of surgery. However, outcomes depend heavily on:
- Adherence to dietary guidelines
- Regular physical activity
- Attendance at follow-up appointments
- Psychological wellbeing and support
Some patients experience weight regain after 2–5 years if dietary habits slip. That’s why the commitment to lifestyle change is non-negotiable.
NHS vs Private Gastric Sleeve — A Comparison
If NHS waiting times are too long or you don’t meet the eligibility criteria, private surgery is an option — but it comes at a cost.
| Factor | NHS Gastric Sleeve | Private Gastric Sleeve (UK) |
|---|---|---|
| Cost | Free | £8,000 – £12,000+ |
| Waiting time | 18 months – 3+ years | 2–6 weeks |
| Eligibility | Strict BMI + co-morbidity criteria | Generally BMI 30+ |
| Tier 3 programme required? | Yes (6–12 months) | No (but assessment still required) |
| Aftercare | NHS follow-up for 2 years + GP long-term | Varies by provider (often 1–2 years) |
| Choice of surgeon | Limited | You choose your surgeon |
| Pros | Completely free; structured pathway | Fast; more flexible eligibility |
| Cons | Very long waits; regional variation | Expensive; aftercare quality varies |
In the UK, gastric sleeve surgery prices in private clinics are often out of reach for many patients, with typical package costs ranging from around £8,000 to £13,000 depending on provider and location.
Common Mistakes and Pitfalls to Avoid
Many patients unintentionally slow down their own journey. Here are the most common errors:
- Not documenting weight loss attempts. Your GP needs evidence that you’ve tried non-surgical methods for at least 12 months. Keep records of every programme, diet, and appointment.
- Assuming your GP will automatically refer you. Some GPs are less familiar with bariatric referral pathways. Come prepared with knowledge of the NICE criteria and your BMI/health data.
- Ignoring the psychological assessment. This isn’t a box-ticking exercise. Bariatric teams need to see that you understand the lifelong commitment. Engage genuinely with the process.
- Dropping out of the Tier 3 programme. Even missing a few sessions can result in being discharged from the programme and having to start again.
- Expecting surgery alone to solve everything. Surgery is a powerful tool, but without dietary and lifestyle changes, weight regain is common.
Who Should Consider NHS Gastric Sleeve — and Who Should Look Elsewhere
Best for:
- Adults with BMI 35+ and at least one obesity-related health condition
- UK residents willing to engage with a structured 6–12 month weight management programme
- Those who cannot afford private surgery and are prepared for a long wait
- Patients committed to lifelong dietary changes and follow-up
Not for:
- People with BMI below 35 without qualifying conditions (unless ethnicity-adjusted thresholds apply)
- Those seeking surgery within weeks — NHS timelines are measured in years
- Anyone unwilling to commit to lifelong vitamin supplementation and dietary changes
- Patients with active untreated eating disorders, severe psychiatric conditions, or substance abuse issues
Final Verdict
Getting a gastric sleeve on the NHS is absolutely possible — but it requires preparation, patience, and persistence. The process involves multiple stages, from your initial GP conversation through a Tier 3 weight management programme to a full multidisciplinary assessment before surgery is even scheduled.
The most important step? **Start now.** The sooner you book that GP appointment and begin documenting your weight loss journey, the sooner the clock starts ticking on a pathway that could take 18 months to 3+ years.
If NHS waiting times or eligibility criteria rule out this route, private surgery is an alternative — but do your research, check the provider’s aftercare programme, and understand the full cost before committing.
Your weight doesn’t define your worth, but if surgery is the right medical decision for your health, you deserve to understand exactly how to access it.
Frequently Asked Questions
Q: Can I get a gastric sleeve on the NHS for free?
A: Yes. If you meet the eligibility criteria set by NICE guidelines, gastric sleeve surgery is fully funded by the NHS. This includes the surgery itself, hospital stay, and follow-up care.
Q: What BMI do I need for gastric sleeve surgery on the NHS?
A: You typically need a BMI of 40 or above, or a BMI between 35 and 40 with a significant obesity-related condition such as type 2 diabetes or obstructive sleep apnoea. In exceptional cases, a BMI of 30–35 may qualify if recent-onset type 2 diabetes is present.
Q: How long is the NHS waiting list for bariatric surgery?
A: Total wait times range from 18 months to over 3 years, depending on your NHS region. This includes the Tier 3 programme (6–12 months) and the surgical waiting list itself.
Q: Is gastric sleeve or gastric bypass better on the NHS?
A: Both are effective. Research suggests gastric bypass may offer slightly better long-term weight loss and diabetes remission for some patients. Your surgeon will recommend the procedure best suited to your individual health profile.
Q: What happens if the NHS rejects my bariatric surgery application?
A: You can ask for a formal explanation, request a review, or seek a second opinion. If you still don’t qualify, private surgery in the UK (£8,000–£12,000) or overseas options are available.
Q: Do I need to lose weight before NHS gastric sleeve surgery?
A: Yes. You’ll need to complete a Tier 3 weight management programme (6–12 months), and many programmes require a 5–10% weight loss. You’ll also follow a liver-shrinking diet 2–4 weeks before surgery.
