You’ve probably Googled teeth whitening and landed on twelve different articles — each one promising the “best” method while quietly ignoring the trade-offs. Here’s the honest version.
Teeth whitening genuinely works. But which method works *best* depends on your stain type, how sensitive your teeth are, your timeline, and your budget. Get it wrong and you risk wasting money on products that won’t move the needle — or worse, using something too aggressive and causing enamel damage that’s difficult to reverse.
This guide covers every major whitening method, the science behind how they work, real safety considerations, and a clear decision framework so you can choose confidently — without consulting twelve more articles after this one.
Whether you’re comparing strips to professional treatment, trying to avoid sensitivity, or researching PAP-based options, you’ll find your answer here.
Table of Contents
Quick Answers:
- What is teeth whitening?** → A bleaching process that removes stains from tooth enamel using peroxide or PAP compounds
- Best for dramatic, fast results?** → In-office professional whitening (30–90 min, dentist-applied)
- Best affordable at-home option?** → OTC whitening strips with 10% hydrogen peroxide
- Does it damage teeth?** → Safe when used correctly; overuse can thin enamel over time
- How long do results last?** → 6 months to 2+ years depending on your habits and method
## What Is Teeth Whitening?
Teeth whitening is a cosmetic dental procedure that lightens tooth enamel by using bleaching agents — primarily hydrogen peroxide or carbamide peroxide — to break down stain molecules. It can reduce both surface (extrinsic) stains and some deeper (intrinsic) discoloration, though effectiveness varies by stain type and method.
Not all tooth discoloration responds the same way. **Extrinsic stains** — caused by coffee, tea, red wine, and tobacco — sit on the surface of enamel and typically respond well to most whitening methods. **Intrinsic stains** — caused by aging, certain medications (like tetracycline), or trauma — are embedded within the tooth structure and are harder to remove, often requiring stronger professional treatments or specialist evaluation.
One critical limitation: **teeth whitening does not work on dental restorations.** Crowns, veneers, bridges, and tooth-colored fillings won’t change shade. If your smile includes restorations, this matters — a mismatch in whiteness between natural teeth and restorations can look uneven. Discuss this with your dentist before starting.
In‑office whitening is usually carried out by an experienced cosmetic dentist in Beverly Hills or a similar cosmetic dental provider, who can assess your stain type and recommend the safest, most effective approach for your teeth.
## How Teeth Whitening Works
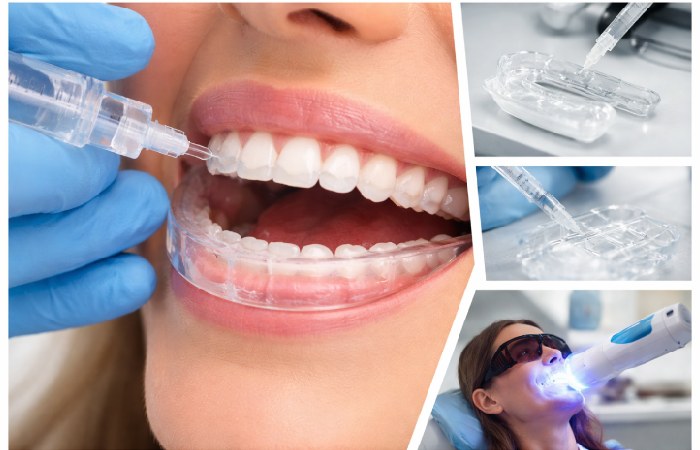
### The Peroxide Science
Most whitening products rely on **hydrogen peroxide (HP)** or **carbamide peroxide (CP)**. Both are bleaching agents — but they work slightly differently.
Hydrogen peroxide penetrates the enamel and reaches the dentin layer below. There, it releases oxygen radicals that react with colored chromophore molecules (the compounds responsible for discoloration) and break them apart. The result: tooth shade lightens.
Carbamide peroxide breaks down into hydrogen peroxide plus urea. It releases its active compound more slowly, which is why it’s used in overnight or extended-wear trays. Lower immediate intensity makes it gentler — but it takes longer to achieve results.
Professional in-office treatments use concentrations of **15–40% hydrogen peroxide**. Over-the-counter products typically use **3–10%**. Higher isn’t always better — concentration affects speed, not the maximum whiteness achievable.
As clinical studies on hydrogen peroxide and enamel permeability published via NCBI/PubMed confirm, peroxide does penetrate beyond enamel, which explains both its effectiveness and the temporary sensitivity it can cause.
### PAP — The Peroxide-Free Alternative
A newer compound, **PAP (phthalimidoperoxycaproic acid)**, is gaining traction — especially among people with sensitive teeth. PAP oxidizes stain molecules without generating free radicals, which is the main mechanism behind peroxide sensitivity.
The result: comparable whitening effectiveness with significantly less sensitivity. PAP products are now available in strips, pens, and professional-grade kits. They’re an excellent option for anyone who has abandoned whitening in the past due to pain.
### Light Activation — Does LED Actually Help?
LED and blue-light devices are marketed as “accelerators” for whitening gel. The evidence is mixed. Light activation can speed up the initial oxidation of peroxide — but the final whitening outcome at 2–4 weeks is often similar with or without light, according to several clinical studies.
Where light *does* add consistent value: in-office laser-activated systems, which use calibrated wavelengths at intensities far beyond what consumer devices deliver. A $30 drugstore LED kit is not the same as a clinical light-activation system.
Bottom line: LED is a nice bonus, not a requirement. Don’t let it be the deciding factor.
## Types of Teeth Whitening Methods
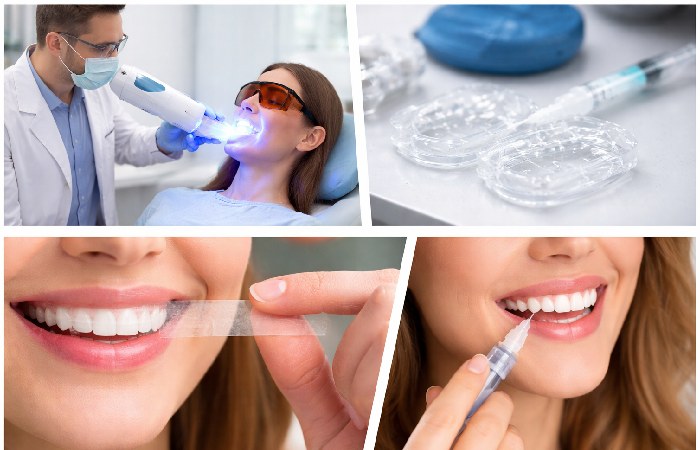
Here’s the full comparison across the five main whitening approaches:
| Method | Avg. Cost | Whitening Results | Time to Results | Sensitivity Risk | Longevity |
|---|---|---|---|---|---|
| In-office professional | $300–$700+ | Dramatic (6–10 shades) | 1 session (30–90 min) | Moderate–High | 1–2 years |
| Dentist take-home kit | $150–$400 | Significant (4–8 shades) | 1–2 weeks | Low–Moderate | 1–2 years |
| OTC whitening strips | $20–$60 | Moderate (2–5 shades) | 1–3 weeks | Low–Moderate | 4–6 months |
| Whitening pen / gel | $15–$40 | Mild (1–3 shades) | Ongoing maintenance | Low | 2–4 months |
| Whitening toothpaste | $5–$20 | Mild (surface only) | Weeks to months | Very low | Ongoing (maintenance) |
### In-Office Professional Whitening
This is the fastest, most dramatic option. A dentist applies a high-concentration peroxide gel (15–40%) and often uses light or laser activation to accelerate the process. Gums and soft tissues are protected with barriers.
A single session typically takes 30–90 minutes and can lighten teeth by 6–10 shades. Results last 1–2 years with proper maintenance.
The downside: cost. In-office whitening typically runs **$300–$700+** depending on location and provider. Post-procedure sensitivity is common for 24–48 hours.
Best for: people who want the fastest possible results with professional supervision.
### Dentist-Prescribed Take-Home Kits
Your dentist takes digital scans or impressions and fabricates custom-fitted whitening trays. You fill them with professional-grade gel (typically 6–16% carbamide or hydrogen peroxide) and wear them at home — usually 30–60 minutes daily for 1–2 weeks.
Results are comparable to in-office treatment over time, though they arrive more gradually. Custom trays provide better gel coverage and less gum irritation than universal-fit OTC trays.
Cost: typically **$150–$400**. These kits also serve as excellent top-up tools after an initial in-office treatment.
Best for: people who want professional-grade results on a flexible schedule.
### OTC Whitening Strips
The most popular at-home option. Thin plastic strips coated with a peroxide gel (typically 6–10% HP) are pressed directly onto the teeth twice daily for 20–30 minutes, usually for 14–21 days.
Strips are effective for mild-to-moderate extrinsic staining. They’re accessible, affordable, and produce noticeable results — 2–5 shades lighter — when used consistently.
The limitation: strips don’t adapt to tooth shape, so coverage can be uneven. The gel also doesn’t reach between teeth. For surface staining on front teeth, they’re excellent. For comprehensive whitening, professional options outperform them.
Best for: budget-conscious users with mild surface staining.
### Whitening Pens and Gels
Brush-on applicators with low-concentration peroxide or PAP. Best used for touch-ups and maintenance between whitening sessions — not as a primary treatment.
Results are subtle. These pens won’t produce a dramatic initial change, but they’re convenient for post-treatment maintenance.
### Whitening Toothpastes and Mouthwashes
Whitening toothpastes work differently — most use mild abrasives to polish surface stains rather than bleaching agents. Some contain low-dose hydrogen peroxide or PAP.
They won’t remove deep staining, but they’re useful for preventing new stain buildup and maintaining results after whitening treatment. Nano-hydroxyapatite (nHAp) toothpastes are an emerging category that both gently brighten and actively **remineralize enamel** — a dual benefit worth considering, particularly after any bleaching treatment.
Best for: daily maintenance; not a standalone whitening solution.
## Is Teeth Whitening Safe?
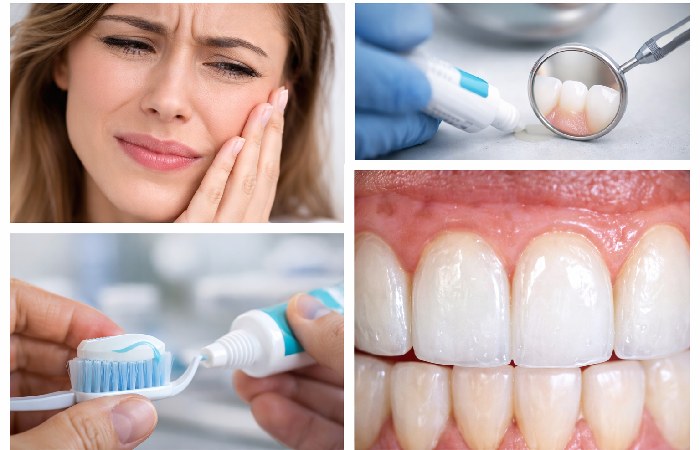
### Common Side Effects
The two most reported side effects are **tooth sensitivity** and **gum irritation.**
Sensitivity occurs because peroxide molecules penetrate enamel and stimulate nerve endings in the dentin layer. It’s almost always temporary — resolving within 24–72 hours after treatment. Using a desensitizing toothpaste containing potassium nitrate before and after whitening significantly reduces discomfort.
Gum irritation typically comes from gel contact. Professional protocols protect gum tissue with barriers; at home, ensure gel stays on teeth only.
### Enamel Safety — The Over-Whitening Risk
This is the most underserved safety topic in mainstream whitening content. **Over-whitening is real.**
Repeated, frequent bleaching — especially at high concentrations — can increase enamel porosity over time and contribute to structural weakening. This doesn’t mean whitening is dangerous; it means there’s a threshold you shouldn’t repeatedly cross.
Practically: don’t whiten more often than your dentist or product instructions recommend. When results plateau (there’s a natural ceiling to whiteness), continuing treatment won’t add benefit — it only adds risk.
According to the American Dental Association’s overview of tooth whitening, whitening products are safe when used as directed, but overuse or unsupervised use of very high concentrations can cause adverse effects.
### PAP vs. Peroxide: Sensitivity Comparison
| Feature | Hydrogen peroxide | PAP |
|---|---|---|
| Mechanism | Free radical oxidation | Oxidation without free radicals |
| Sensitivity | Moderate–high | Low–very low |
| Effectiveness | High | Comparable to low–mid hydrogen peroxide |
| Speed | Faster (at higher concentrations) | Moderate |
| Best for | Fast results; tolerant users | Sensitive teeth; first-time users |
| Availability | Widely available (OTC + professional) | Growing; OTC + professional kits available |
If you’ve experienced pain with whitening before, PAP-based products are worth switching to.
## How Long Does Teeth Whitening Last?
### Results by Method
| Method | Typical longevity |
|---|---|
| In-office professional | 12–24 months |
| Dentist take-home kits | 12–18 months |
| OTC strips | 4–6 months |
| Whitening pens | 2–4 months |
These ranges assume consistent oral hygiene and lifestyle. Heavy coffee, tea, red wine, or tobacco consumption shortens results at every level.
### How to Maintain Your Results
1. Follow the 48-hour white diet** after any whitening session — avoid chromogen-rich foods and drinks (coffee, tea, berries, soy sauce, red wine). Enamel is more porous immediately post-treatment.
2. Use a whitening or nHAp toothpaste** daily to prevent new stain accumulation and support enamel remineralization.
3. Drink dark liquids through a straw** to minimize contact with enamel.
4. Schedule touch-up treatments** — a single whitening pen session or a 1-week strip cycle every 3–6 months maintains results without the full cost of retreatment.
5. Quit smoking.** Tobacco staining is aggressive and largely reverses whitening results within months.
Post-treatment guidance from NHS recommendations on tooth whitening care
supports the same approach: minimize contact with staining agents immediately after treatment and maintain regular oral hygiene.
## Common Mistakes to Avoid
- Using OTC products on damaged teeth without a dental check.** If you have untreated cavities, gum disease, or enamel erosion, whitening gel can penetrate damaged areas and cause significant pain or accelerate the problem. Get a dental exam first.
- Chasing results past the whitening plateau.** There’s a natural shade ceiling based on your tooth genetics. Once you’ve reached it, additional whitening won’t add further brightness — it just increases enamel exposure risk. Stop when you’ve hit your baseline maximum.
- Skipping the 48-hour post-treatment window.** The most common reason whitening results fade fast is consuming staining foods before the enamel has re-hardened. Two days of care dramatically extends your results.
- Using activated charcoal products.** Despite marketing claims, activated charcoal is highly abrasive and has no reliable evidence of whitening effectiveness. It can physically scratch enamel and increase sensitivity over regular use.
- Assuming whitening works on all teeth.** If your discoloration is caused by tetracycline antibiotics, fluorosis, or trauma — standard whitening will have limited effect. These cases require specialist evaluation and potentially different interventions (e.g., veneers, KöR deep whitening protocol).
## Who Is Teeth Whitening For — And Who Should Avoid It
### Best For:
- Adults with healthy enamel and predominantly extrinsic staining (coffee, tea, wine, tobacco)
- People with natural teeth (no significant restorations in the smile zone)
- Those who want a clinically safe confidence boost for an upcoming event or milestone
### Proceed With Caution:
- Sensitive teeth:** Try PAP-first or dentist-supervised low-concentration kits; avoid aggressive OTC products
- Mild intrinsic staining:** Professional treatment may help; manage expectations
- Existing dental work in the smile zone:** Discuss the color match issue with your dentist before whitening natural teeth
### Not Recommended For:
- Pregnant or nursing individuals (out of precaution; insufficient safety data)
- Children and adolescents under 18
- Anyone with untreated tooth decay, gum disease, or significant enamel erosion
- Teeth severely stained by tetracycline (requires specialist-level intervention)
- Users of crowns, veneers, or fillings who expect uniform whitening (won’t change restorations)
## Final Verdict — Choosing the Right Whitening Method

Here’s the decision framework:
| Your situation | Best approach |
|---|---|
| Want the fastest, most dramatic result | In-office professional whitening |
| Want professional results on a budget with flexibility | Dentist take-home kit |
| Mild surface staining, limited budget | OTC whitening strips (10% hydrogen peroxide) |
| Sensitive teeth, first-time whitener | PAP-based strips or dentist-supervised low-dose kit |
| Maintenance after whitening | Whitening or nHAp toothpaste plus occasional whitening pen |
| Severe intrinsic staining or dental restorations | Consult a dentist before any whitening attempt |
No single method wins for everyone. The best choice is the one that fits your stain type, sensitivity tolerance, timeline, and budget. When in doubt — especially if you haven’t had a dental check in over a year — get one before you start. Your dentist can spot contraindications and recommend the appropriate concentration and method.
## Frequently Asked Questions
Q1: Is teeth whitening safe for enamel?
A: Yes, when used as directed. Properly used whitening products don’t permanently damage enamel. Overuse — particularly of high-concentration products used more frequently than recommended — can increase enamel porosity over time. Follow product instructions and consult a dentist if you’re unsure.
Q2: How long do whitening results last?
A: Results vary by method. In-office professional whitening typically lasts 12–24 months; OTC strips average 4–6 months. Longevity depends heavily on diet and lifestyle — frequent coffee, tea, wine, or tobacco use shortens results significantly.
Q3: What is the difference between hydrogen peroxide and PAP whitening?
A: Hydrogen peroxide whitens via free radical oxidation, which is effective but can cause sensitivity by penetrating dentinal tubules. PAP (phthalimidoperoxycaproic acid) oxidizes stains without free radicals, producing comparable whitening with significantly less sensitivity. PAP is the preferred choice for people who have experienced discomfort with traditional peroxide products.
Q4: Does teeth whitening work on crowns or veneers?
A: No. Whitening agents do not change the color of dental restorations — crowns, veneers, bridges, or tooth-colored fillings are unaffected. Whitening natural teeth while you have visible restorations may create a color mismatch. Discuss this with your dentist before starting.
Q5: Can I whiten my teeth if I have sensitive teeth?
A: Yes, with the right product. PAP-based whitening products are specifically formulated to minimize sensitivity. Alternatively, a dentist-prescribed low-concentration carbamide peroxide kit with desensitizing agents (potassium nitrate, fluoride) is a safe approach. Avoid aggressive OTC products or prolonged wear times.
Q6: How often can I whiten my teeth safely?
A: Follow manufacturer guidelines — typically once every 3–6 months for in-office or strip treatments. Daily whitening toothpaste is fine for ongoing maintenance. Don’t repeat clinical-strength treatments more than twice per year without dental supervision. Your teeth have a natural whiteness ceiling; exceeding treatment frequency past that point adds risk without additional benefit.
Disclaimer
This guide is for general information and does not replace professional dental advice, diagnosis, or treatment. Teeth whitening is not suitable for everyone, and results and risks can vary. Always consult a licensed dentist about your specific teeth, existing dental work, and any sensitivity before starting, changing, or repeating a whitening treatment.”
