Most people who are struggling emotionally aren’t in crisis. They’re not diagnosably ill. They’re just overwhelmed, burned out, or stuck — and not quite sure whether what they’re feeling is “serious enough” to see a therapist.
That gap has a name: the missing middle of mental healthcare. And it’s where a mental health coach operates.
This guide cuts through the confusion. You’ll learn exactly what a mental health coach does, how they differ from therapists and psychologists, what credentials to look for, how much to expect to pay, and — critically — how to know which type of professional your situation actually calls for.
Table of Contents
Key Answers Up Front
- What is a mental health coach? A trained professional who helps clients build resilience, manage stress, and achieve emotional wellbeing goals — without diagnosing or treating clinical conditions.
- Coach vs. therapist: Therapists treat diagnosed disorders and heal the past; coaches help non-clinical clients optimize the present and build future-focused skills.
- Does a coach need a degree? No state license is required, but reputable coaches hold ICF or NBHWC credentials. Always verify.
- How much does it cost? Typically 75–150 per session — compared to 150–250 for licensed therapy.
- Is coaching covered by insurance? Rarely. Therapy often is. This is a meaningful practical difference.
What Is a Mental Health Coach?

A mental health coach is a trained professional who supports clients in developing psychological resilience, managing stress, improving emotional regulation, and working toward personal wellbeing goals. Unlike licensed therapists or psychologists, they do not diagnose mental health conditions, prescribe medication, or treat clinical disorders.
The distinction matters more than most people realize. Mental health coaching works by helping clients identify patterns, set actionable goals, and build coping skills — not by exploring trauma or providing clinical intervention. Think of it as the difference between a personal trainer and a physiotherapist: both support physical health, but their scope and methods are fundamentally different.
According to the International Coaching Federation (ICF), supporting mental wellbeing through coaching doesn’t mean crossing into therapy — it means equipping clients with evidence-based tools for resilience and self-management.
The Core Distinction: Mental Health Coach vs. Licensed Therapist
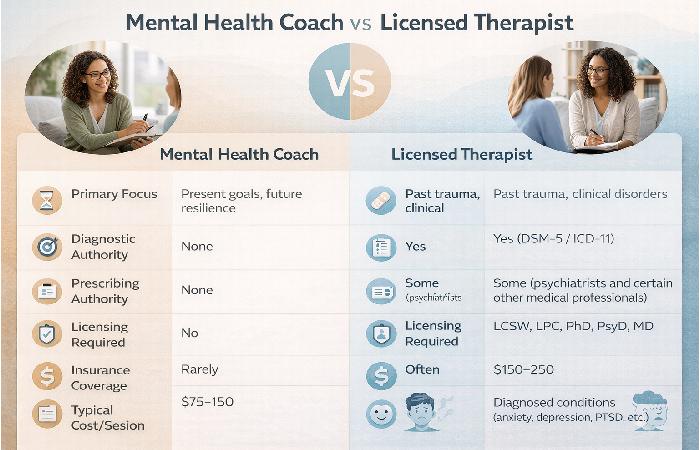
This is the question the SERP is flooded with — and for good reason. Conflating the two roles can lead to real harm. Here is the actual difference.
Scope of Practice: Healing the Past vs. Optimizing the Future
| Dimension | Mental Health Coach | Licensed Therapist |
|---|---|---|
| Primary focus | Present goals, future resilience | Past trauma, clinical disorders |
| Diagnostic authority | None | Yes (DSM-5 / ICD-11) |
| Prescribing authority | None | Some (psychiatrists and certain other medical professionals) |
| Licensing required | No (state-specific) | Yes — LCSW, LPC, PhD, PsyD, MD |
| Insurance coverage | Rarely | Often |
| Typical cost/session | 75–150 | 150–250 |
| Crisis intervention | Not equipped | Yes |
| Best for | Sub-clinical stress, burnout, life transitions | Diagnosed conditions (anxiety, depression, PTSD, etc.) |
A mental health coach also sits in a different space from traditional life coaching. While many life coaches focus on goals, career, or performance, a mental health coach centers specifically on emotional wellbeing, stress management, and psychological resilience for people who are not seeking clinical treatment. This makes mental health coaching a bridge between therapeutic care and more general personal development work.
The Clinical Line: Diagnosis, Medication, and Crisis Intervention
A mental health coach cannot — and should not attempt to:
- Diagnose any mental health condition (anxiety disorder, PTSD, depression)
- Recommend, adjust, or discuss psychiatric medication
- Provide crisis support or safety planning for suicidal ideation
- Treat trauma using clinical modalities (EMDR, CBT administered therapeutically)
This isn’t just an ethical boundary. In many jurisdictions, providing psychotherapy without an appropriate license may be illegal and is widely considered unethical. The line is drawn precisely here: a coach supports wellness; a therapist treats illness.
Why Demand for Mental Health Coaches Is Exploding
The surge in coaching isn’t a trend. It’s a response to a supply-and-demand crisis in mental healthcare that isn’t going away.
The Global Access Gap
- According to SAMHSA’s 2024 National Survey on Drug Use and Health, about 1 in 4 U.S. adults experienced any mental illness in the past year.
- The CDC reports that 1 in 5 U.S. adults has been diagnosed with an anxiety disorder at some point.
- The U.S. faces a severe shortage of licensed mental health providers, with nearly half of counties lacking a single psychiatrist (HRSA estimates).
The result: tens of millions of people who need support — but not necessarily clinical treatment — have nowhere practical to turn. Long waitlists, high out-of-pocket costs, and insurance barriers push them toward other options.
Mental health coaching fills a real gap for people who are sub-clinical but struggling: managing chronic work stress, navigating a difficult life transition, building coping skills after a difficult year, or simply trying to sustain their mental fitness the way they sustain their physical fitness.
What Does a Mental Health Coach Actually Do?

A session with a mental health coach looks quite different from a therapy appointment. There’s no diagnostic intake, no treatment plan in the clinical sense. The work is goal-directed, skills-focused, and largely future-oriented.
Behavioral Activation and Goal Setting
One of the primary tools coaches use — borrowed from cognitive-behavioral research — is behavioral activation: identifying activities and behaviors that improve mood, energy, and motivation, then systematically building them into a client’s routine.
This is not therapy. It’s structured habit-building with professional support and accountability. A coach might help a client:
- Identify the specific stressors driving their anxiety or low energy
- Design a realistic weekly structure that protects recovery and rest time
- Build a set of micro-habits (5-minute daily practices) for emotional regulation
- Track mood and energy patterns to surface triggers and depletion cycles
Mindfulness, Resilience, and Stress Management Frameworks
Many mental health coaches are trained in evidence-informed frameworks, including:
- Motivational Interviewing (MI): A collaborative conversation approach that strengthens a client’s own motivation to change, rather than prescribing what to do.
- Mindfulness-Based Stress Reduction (MBSR): Attention-training practices that reduce the physiological and psychological impact of chronic stress.
- Acceptance and Commitment Coaching (ACC): Helping clients clarify their values and act in alignment with them — even in the presence of difficult thoughts or feelings.
These are coaching adaptations of clinically-developed frameworks, used without clinical assessment or treatment intent. The distinction is meaningful.
Does Mental Health Coaching Actually Work?
This deserves an honest answer. The evidence base for mental health coaching is growing but less established than for licensed psychotherapy. That’s not a reason to dismiss coaching — it’s context for where it fits.
Evidence-Based Outcomes for Non-Clinical Populations
For sub-clinical populations — people experiencing stress, mild burnout, or general emotional difficulty without a formal diagnosis — coaching research shows meaningful improvements in:
- Goal attainment and self-efficacy
- Perceived stress and resilience
- Emotional regulation and mood stability
Recent ICF survey data suggests that many coaches feel they need additional training to effectively support mental wellbeing — underscoring both the rapid growth of the field and the importance of credential verification before hiring.
For clinical conditions — diagnosed depression, anxiety disorders, PTSD, eating disorders — the evidence does not support coaching as a standalone intervention. These conditions require licensed professional treatment. A coach who positions themselves otherwise is operating outside their competency.
How to Choose a Mental Health Coach: Credentials and Red Flags
There is no universal licensing requirement for mental health coaches in the United States. That’s both a feature (lower barriers to access) and a risk (quality varies significantly). Here’s how to navigate it.
Understanding NBHWC vs. ICF Credentials

Two credentialing bodies set the standard most worth knowing:
| Credential | Issuing Body | Focus | Key Requirements |
|---|---|---|---|
| NBC-HWC | National Board for Health & Wellness Coaching (NBHWC) | Health behavior change, integrated with clinical care | 75+ client hours, approved training, board exam |
| ICF-ACC | International Coaching Federation | General coaching (entry level) | 60+ training hours, 100+ client hours |
| ICF-PCC | International Coaching Federation | Professional coaching | 125+ training hours, 500+ client hours |
| ICF-MCC | International Coaching Federation | Master certified coaching | 200+ training hours, 2,500+ client hours |
The NBHWC credential is particularly relevant for mental health coaching because it requires integration with healthcare settings and explicit scope-of-practice training.
5 Red Flags Your Coach Is Overstepping
These aren’t edge cases. Watch for them:
- Diagnosing without a license — Any coach who tells you that you have depression, an anxiety disorder, or PTSD is practicing medicine without a license.
- Discouraging therapy or medication — A reputable coach works alongside clinical care, not against it.
- Promising clinical outcomes — “I’ll cure your anxiety” or “You won’t need your therapist after this” are disqualifying statements.
- No credentials or training disclosure — A professional will clearly state their training background and what they are not qualified to do.
- Taking on clients in active crisis — If you’re experiencing suicidal thoughts or severe psychiatric symptoms, a coach is not the appropriate first responder. In the U.S., call or text 988 (Suicide & Crisis Lifeline) or contact local emergency services.
How to Choose a Mental Health Coach: 5-Point Checklist
Before you commit, run through this quick checklist:
-
Verify credentials and training: Look for ICF or NBC-HWC certification, and ask about their training hours and supervision.
-
Confirm scope and referral plans: Ask what sits outside their scope and how they handle clients who need clinical care.
-
Assess fit in a consult: Use a free or low-cost intro session to see if their communication style and approach feel safe and effective for you.
-
Ask about methods and structure: Have them explain how sessions work, what frameworks they use, and how they measure progress.
-
Clarify pricing and logistics: Understand their fees, packages, session frequency, and cancellation policy before you start.
Cost and Accessibility: A Transparent Comparison
Mental health coaching is generally less expensive than licensed therapy — and for many people, that cost difference is the deciding factor.
| Service | Typical Cost Per Session | Insurance Coverage | Average Waitlist |
|---|---|---|---|
| Mental Health Coach | 75–150 | Rarely covered | Low (often immediate) |
| Licensed Therapist (LCSW/LPC) | 150–250 | Often covered | 4–12 weeks |
| Psychologist (PhD/PsyD) | 200–350 | Partially covered | Weeks to months |
| Psychiatrist | 300–575 (initial) | Often covered | Often months |
Therapy cost ranges per Octave/TherapyRoute 2025 provider analysis. Coaching cost ranges reflect coaching directory market data.
The access advantage is real. For someone managing workplace burnout or a difficult life transition — without a clinical diagnosis — a mental health coach may offer timely, affordable support that simply isn’t accessible through the clinical system right now.
The Future: Hybrid Care and AI-Augmented Coaching
The most important shift in 2026 isn’t a new coaching technique. It’s the emergence of hybrid care models in which coaches work alongside licensed therapists within coordinated care frameworks.
In these models:
- A therapist handles clinical diagnosis, trauma processing, and crisis intervention
- A coach provides between-session accountability, goal-setting work, and skill reinforcement
- Both professionals communicate and align on the client’s overall care plan
Major employers and digital health platforms are integrating this structure to address the mental health access gap at scale. Understanding where coaching ends and clinical care begins becomes more — not less — important as integration increases.
Common Mistakes to Avoid When Choosing a Mental Health Coach
- Choosing based on social media presence alone. A large Instagram following is not a credential.
- Using coaching to avoid clinical treatment. If a licensed professional has recommended therapy or medication, coaching is not a substitute — it may be a complement, but only with your provider’s knowledge.
- Skipping the credential check. Ask directly: “What credentials do you hold? What certifying body issued them? What are you not qualified to help with?” A good coach welcomes these questions.
- Expecting crisis support. Coaches are not crisis counselors. For urgent needs, contact 988 or go to an emergency room.
Who a Mental Health Coach Is — and Isn’t — For
A mental health coach is a strong fit if you:
- Are experiencing sub-clinical stress, burnout, or emotional fatigue without a formal diagnosis
- Want accountability and structure around building emotional resilience habits
- Are already in therapy and want between-session support and skill practice
- Are navigating a life transition (divorce, career change, loss) without acute psychiatric symptoms
- Prefer a goal-directed, action-oriented approach to mental wellbeing
See a licensed therapist or psychiatrist instead if you:
- Have a diagnosed mental health condition (depression, anxiety disorder, PTSD, OCD, bipolar disorder)
- Are experiencing symptoms that significantly impair daily functioning
- Have a history of trauma that needs clinical processing
- Are currently in psychiatric crisis or having thoughts of self-harm
- Have been advised by a healthcare provider to seek clinical mental health treatment
Final Verdict: Where Mental Health Coaching Fits
The mental health system has long operated in binary terms: either you’re “well enough” to need nothing, or “sick enough” to need a clinician. That binary leaves millions of people in the middle — struggling, but not in crisis; needing support, but not needing treatment.
A mental health coach serves that middle. When chosen carefully — with verified credentials, clear scope limits, and appropriate referral pathways — coaching is a legitimate and valuable part of the broader mental wellness ecosystem.
It is not therapy. It does not replace clinical care. But for the right person at the right moment, it may be exactly what moves the needle.
Frequently Asked Questions
Q: Can a mental health coach diagnose anxiety or depression?
A: No. Mental health coaches are not licensed clinicians and cannot diagnose any mental health condition. Diagnosis requires a licensed professional — psychologist, psychiatrist, or licensed therapist. A coach who suggests you have a specific disorder is overstepping their scope of practice.
Q: What is the difference between a life coach and a mental health coach?
A: The terms overlap significantly. A life coach typically focuses on goals, performance, and life direction; a mental health coach specifically focuses on emotional wellbeing, stress management, and psychological resilience. Neither can diagnose or treat clinical conditions. Mental health coaches typically have more specialized training in wellness frameworks such as mindfulness-based approaches and motivational interviewing.
Q: Is mental health coaching covered by insurance?
A: In most cases, no. Unlike licensed therapy, coaching is generally not reimbursable under standard health insurance plans. Some employers offer coaching through EAP (Employee Assistance Programs) or corporate wellness benefits. Always verify coverage before starting.
Q: How much does a mental health coach cost per session?
A: Most mental health coaches in the United States charge between 75 and 150 per session. Package pricing often reduces the per-session rate. This is generally lower than licensed therapists (often 150–250 per session), though insurance may significantly offset therapy costs if you have coverage.
Q: Does a mental health coach need a degree or license?
A: No state license is legally required in most U.S. jurisdictions. However, reputable coaches hold credentials from recognized bodies such as the ICF (International Coaching Federation) or NBHWC (National Board for Health & Wellness Coaching). Always ask for credentials and verify them before committing to work with a coach.
Q: Can a mental health coach work with someone who has PTSD?
A: With significant caution. PTSD is a clinical diagnosis that typically requires trauma-focused therapy — such as EMDR or Trauma-Focused CBT — delivered by a licensed clinician. A coach should not attempt trauma processing. A coach might support between-session skill work alongside a therapist treating PTSD, but only with appropriate clinical oversight in place.